On February 21st I was 27 weeks, 3 days pregnant. It had been a blissfully easy, healthy pregnancy. No morning sickness. Good energy levels. My OB sung my praises for eating right and keeping up with my regular exercise routine. I was truly enjoying being pregnant this second time around. I woke up that morning around 5am concerned that I hadn’t felt the baby move all night. I started counting kicks, and finally felt a series of kicks from 6-6:30am. I dismissed my concern as being a neurotic pregnant woman, and got up and got ready for work.
We had a lunch meeting with one of our contact lens reps that day. At lunch I started noticing a lack of fetal movement again. I called my OB’s office and was seen that afternoon at 3:15pm. They performed a fetal non-stress test. Everything came out normal. The baby was moving again, I wasn’t having any contractions, and I was due back for my 28 week visit in five days. Not much could happen before then, right? Wrong.
That evening at 7:04pm I started having contractions. They were brief at first, but each contraction became progressively longer and more intense. They started happening every 5 minutes. Then they were every 3. After about 20 minutes, I called my OB’s office again and spoke to the doctor on call. She said it was “probably nothing” but she would go ahead and meet me at the hospital where they would likely give me something to “calm my uterus down.” Blake was concerned. I rarely complain about how I feel, so he knew something was up. We called our neighbor to come stay with Noah (who was already in bed) and Blake drove me to Parker Adventist Hospital. The trip there only took about 15 minutes, but it felt like an eternity. My contractions were coming every few minutes and getting stronger and more intense. Something was wrong. This wasn’t normal, and we were both nervous.We got to the hospital just before 8pm. Blake dropped me off at the door, and I checked in while he parked the car. I was shown to a triage room to gown up and leave a urine sample. By the time I got out of the bathroom Blake was already in the room waiting. His belt had just broken and he was trying to see if he could fix it. He couldn’t.
A few minutes later, a nurse came in. She wanted to swab my cervix to do a fetal fibronectin lab. She went to swab my cervix, but couldn’t find it. She hustled out of the room, and the OB came in with her a few moments later. The OB took a look and then her expression turned grim. “Oh, man. You’re already 7cm dilated,” she said. “Can you stop the labor?” I asked. “We’ll do what we can to slow it down,” she assured me. I tried to hold back tears. “Will my baby be ok?” The OB looked uncertain and said, “We’re going to do what we can to help.” This was not the answer I wanted to hear. My thoughts quickly turned to what the future was going to look like for our family. Would we be able to handle the loss of this child? And if this baby lived, would she be normal? Visions of a special needs child in a wheelchair flashed through my mind. “Oh God. Please let everything be ok,” I prayed silently but fervently. When I could finally bring myself to look at Blake, it broke my heart. His face was white. He looked as frightened as I felt. “Call my mom. Ask her to pray,” I told him.
From that point forward it was a blur. There was a nurse giving me a steroid shot in my backside. “This is to speed up the baby’s lung development,” they told me. They inverted my bed so my head was below my feet to take the pressure of my cervix. Then they put an IV line in and inserted a catheter (an empty bladder puts less pressure on the uterus). They gave me magnesium (“To protect the baby’s brain”) and antibiotics (since I tested positive for Group B Strep in my last pregnancy) intravenously. They dimmed the lights to help me relax. They offered me an epidural at some point in there. “Will it slow down my labor?” I asked. “No, not at this point,” they replied. So I declined it, thinking to myself, “If for some reason this baby doesn’t make it, I want to feel the pain of birth before I feel the pain of loss.” For about 20 minutes my contractions lessened in intensity and came less frequently. This all had happened while we were still in the triage room. My OB sat by the bed and told me that if I were to deliver sometime in the next four days, my baby would have to be transferred to the NICU at University hospital. Parker didn’t take babies younger than 28 weeks. She noted that my contractions had let up and wondered if I could be transferred to University. I told her there wouldn’t be enough time. My contractions started picking up again. This time they were incredibly painful. I told my OB and the nurses, they had me roll onto my left side to help me relax. Blake had been holding my hand for quite sometime at this point, and gave it a reassuring squeeze. They tried talking me through it, but then I felt the baby moving down the birth canal. “The baby’s coming! I can feel her coming!” I told everyone.
When the doctor felt the baby’s head, she knew I was serious. A team of about eight nurses seemed to appear out of thin air. Because we were still in the triage room, they had to roll me down the hall to a delivery room. I was feeling the need to push but they instructed me to wait. They got my bed in position and dimmed the lights again. They had no sooner brought my bed up (I was still inverted) and got my feet into the stirrups when I couldn’t hold it in any longer. I gave one big push, and out came the baby. Harper Elizabeth was born at 10:04pm, completely contained in her amniotic sac. We would later learn that this was very rare, especially in a natural birth (“The first time I’ve seen it in my 13 years of practice,” a neonatal nurse practitioner told us). To be born inside the unbroken amniotic sac is called an en caul birth. Throughout history in many cultures, being born en caul was a sign that the child was destined for greatness.
Harper cried when she was born. I took this as a sign that she would be ok. I didn’t even get to see her up close for several minutes. As soon as she was born, they whisked her away and started working on her. She weighed 1163 grams (2lb 9oz) and was 15 inches long. A nurse came and asked for Blake’s cell phone to snap a picture before she was intubated. Her APGAR score at birth was 6, and at five minutes it was 8. This was remarkable, as she wasn’t intubated until 7 minutes of life. They say Denver babies never make a perfect 10 due to the altitude.
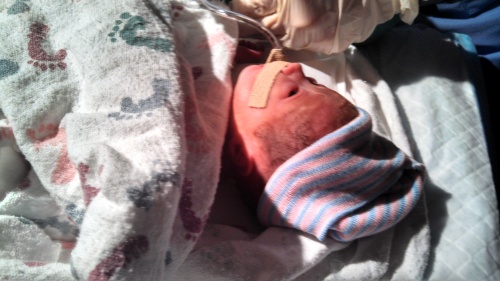
After some time, they rolled Harper’s bassinet over to my bedside. “Would you like to touch her? You can touch her before we take her to the NICU,” a nurse offered. I reached over and touched her tiny little hand. Blake touched her too. Blake went with her to the NICU, at my insistence. Suddenly the room was empty and quiet. The room was dark, as no one had turned the lights back up, and I was just sitting there alone and scared. I was too numb to cry or truly feel the depth of all the emotions in my heart at that moment. I suddenly had a case of shivers, even though I wasn’t cold. I was still in shock.
At some point during the whole process Blake had managed to notify our family, some of our church friends, and our workplaces. Blake’s parents were already on their way to take care of Noah and relieve our neighbor. My parents were coming first thing next morning (they had just driven back to Steamboat from Denver earlier that day). My friend Grace had texted to ask if everything was ok. I called her back and told her what happened. As soon as she found out Harper was being transferred and Blake was going with her, she told me she was coming to stay with me that night. I didn’t want to inconvenience my dear friend (who happened to be 9 months pregnant at that time), and insisted I was fine to be alone. But I wasn’t. I didn’t know it at the time, but I really needed her that night. It was the scariest night of my life, and I’m so glad she was there.
After awhile, maybe 30 minutes or so, a nurse came in to get me cleaned up. Blake came back as well. I found it surprisingly easy to walk to the bathroom without an epidural. She got me changed, and took me in a wheelchair to the NICU with Blake. They wheeled me up to Harper’s bedside. I got to touch her again and look at her tiny little body beneath all the tubes and wires. The neonatologist came and talked to us. He mentioned surfactant and a ventilator and said some other things I was too shell-shocked to remember. The nurse who wheeled me in offered to take me to my room, but I wanted to wait until the transport team came for Harper. I didn’t know if that would be the last time I would get to see my baby girl.
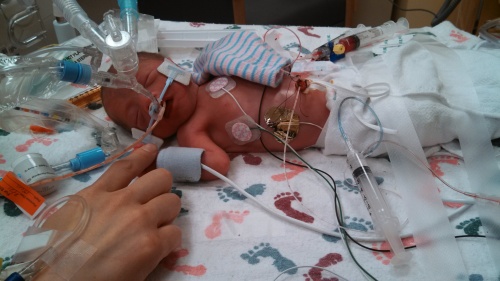
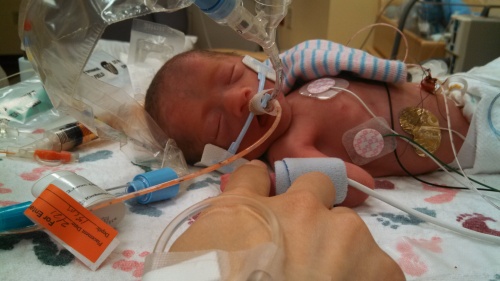
After about half an hour, they took me to my room where Grace was waiting for me. Blake got Harper’s birth certificate paperwork filled out while we waited for Harper to be transferred.

Eventually the transport team stopped by my room so I could say one last goodbye to her through the plastic box, and then they were off. Blake also left to head to University and make sure Harper would be ok. By this time it was about 1:00am. I asked for a pump. There was little to do besides wait to be discharged. And pump. Grace and I talked, and she comforted me with stories of preemies she knew about who were now happy and healthy children. She told me that Harper’s weight was promising and that a recent lecture she had attended had said babies with a weight like Harper’s were very unlikely to develop retinopathy of prematurity. We tried to get some sleep, but I was texting Blake and pumping and ended up getting very little rest. Bless Grace’s heart, she parked her 37-weeks pregnant self on the terribly uncomfortable sleeper sofa and was a reassuring presence to me all night. She even brought me snacks, slippers, and a robe.
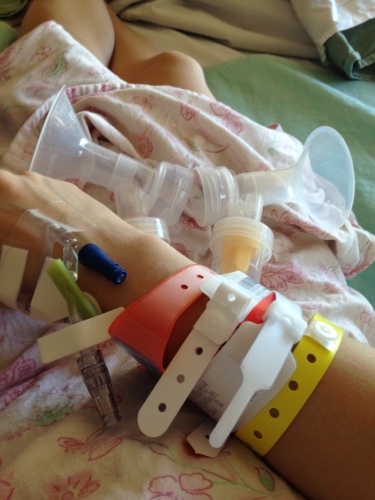
The next morning my OB came back in to check on me. She could tell I was anxious to get out of there and see my baby, so she got my discharge paperwork started. Grace and I ordered breakfast. Blake was back at the NICU seeing Harper, but was coming to pick me up afterward. A lady came by to do a hearing screening and looked confused. “Where’s the baby?” she asked. She looked embarrassed and murmured something apologetic after I explained what happened. Grace spent all morning on the telephone hunting down a Medela Symphony pump for me. Blake came and gave us an update on Harper. They were able to take her off her ventilator and transition her to CPAP. She got a second dose of surfactant that morning. She was on a 9-1-5 care schedule, and we would be able to make it to her 1:00 cares after being discharged. Finally, around 11:00am the nurse was ready to walk us out.
Being discharged from the hospital without a baby was difficult. I had somehow managed to keep it together up until that point, but when we started walking down the hall to leave, I couldn’t stop the tears from streaming down my face. Not two years prior, I was leaving that same hospital with a beautiful, healthy baby boy. Now walking out without my new daughter, feeling so uncertain about her future, just reminded me of how different the situation was this time. The grief hit me like a ton of bricks.
Thus began our 60 day NICU journey, which is another story in itself. They never did find a reason for my preterm labor. The pathology labs on my placenta and umbilical cord, and a post-partum ultrasound showed nothing abnormal. All I can say is that we had an amazing support system throughout all of this. I don’t know what we would have done without everyone’s kindness and prayers. God was faithful to see us through this difficult time and keep our baby girl healthy. It’s still too fresh in my memory to look back on this time without stirring up some raw emotions, but one day I will be able to share this story with Harper about her dramatic entry into the world and her remarkable start in life, and we will marvel at how far she’s come.
 1. I mentioned Dr. Brown’s bottles in my NICU essentials post. It was what our nurses recommended for reducing reflux, and Harper never did have an issue with reflux or spitting up. 4oz bottles will be plenty big in the beginning. Harper started on a preemie nipple when she was first learning to take a bottle, but by the time she was discharged she had graduated to a level 1 nipple..
1. I mentioned Dr. Brown’s bottles in my NICU essentials post. It was what our nurses recommended for reducing reflux, and Harper never did have an issue with reflux or spitting up. 4oz bottles will be plenty big in the beginning. Harper started on a preemie nipple when she was first learning to take a bottle, but by the time she was discharged she had graduated to a level 1 nipple..




